POTS Specialist in Burbank – Integrative POTS Treatment
Navigating POTS Syndrome with a POTS Specialist Burbank Los Angeles
If you are looking for a POTS specialist in Burbank, Dr. Cynthia Thaik provides integrative and holistic care for individuals with Postural Orthostatic Tachycardia Syndrome (POTS). As an experienced POTS specialist in Burbank, she focuses on identifying the root causes of autonomic dysfunction and, in turn, creating personalized treatment plans that support cardiovascular health, nervous system balance, nutrition, and lifestyle improvements.
POTS affects millions of people, with approximately 3 million Americans impacted before COVID-19 and an estimated 6 million since the pandemic began. While anyone can develop POTS, about 75% of patients are women between the ages of 15 and 50. Symptoms may be triggered by pregnancy, surgery, trauma, or viral infections such as mononucleosis, Lyme disease, or COVID-19.
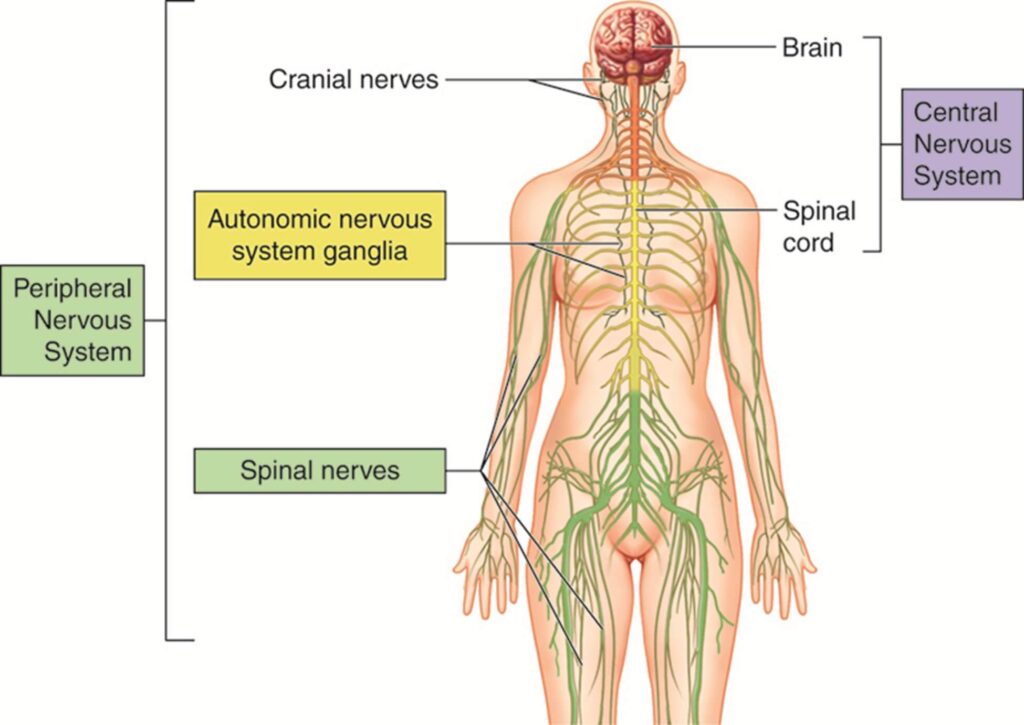
POTS is a type of dysautonomia, meaning the autonomic nervous system—responsible for vital functions such as heart rate, blood pressure, and breathing—does not function properly. As a holistic cardiologist practicing in Los Angeles, Dr. Cynthia Thaik, MD, and the staff at Holistic Healing Heart Center have seen many patients seeking care from a POTS specialist Burbank Los Angeles for adrenal fatigue–related POTS symptoms. We believe in taking a whole-body approach to evaluating POTS, focusing on integrative strategies commonly recommended by a POTS specialist in Burbank, to help patients achieve optimal health and long-term wellness.
POTS) Postural Orthostatic Tachycardia Syndrome Disorder Symptoms – POTS Specialist Burbank Los Angeles
Symptoms of Postural Orthostatic Tachycardia Syndrome (POTS) can differ greatly from one person to another, which can make the condition difficult to diagnose and treat effectively. Understanding these symptoms is key — it helps you recognize when something isn’t right and when it’s time to reach out to your healthcare provider for proper evaluation and support.
Postural orthostatic tachycardia syndrome (POTS Disorder Symptoms) is a condition marked by orthostatic intolerance (OI), where insufficient blood returns to the heart upon standing, contributing to POTS heart disease symptoms. In healthy individuals, blood vessels tighten to maintain blood flow to the brain, but in people with OI this response is impaired, leading to dizziness, lightheadedness, fatigue, brain fog, palpitations, and occasional fainting. Factors such as dehydration, low blood pressure, nervous system disorders, and certain medications can worsen symptoms, which is why care from a trusted POTS specialist Burbank is important. Support from an experienced POTS specialist Burbank helps patients better understand their condition and manage daily symptoms effectively. Let’s review the definition of POTS. Each word of “postural orthostatic tachycardia syndrome” has a meaning:
- Postural: Because POTS is related to body position, symptoms are often triggered by postural changes, particularly standing up.
- Orthostatic: As a result of standing upright, people with POTS often experience symptoms when standing or sitting up for prolonged periods.
- Tachycardia: In POTS, the heart rate may rise above 100 beats per minute, particularly upon standing or changing positions.
- Syndrome: POTS is a syndrome defined by a group of symptoms that occur together and affect both the cardiovascular and nervous systems. These symptoms may include rapid heartbeat, lightheadedness, fatigue, and other issues that can significantly impact quality of life.
Postural orthostatic tachycardia syndrome (POTS) is a blood circulation disorder characterized by two factors:
- A specific group of symptoms that frequently occur when standing upright.
- A heart rate increase from horizontal to standing (or as tested on a tilt table) of at least 30 beats per minute in adults, or at least 40 beats per minute in adolescents, measured during the first 10 minutes of standing.
Postural Orthostatic Tachycardia Syndrome (POTS) is a complex POTS Heart Disease disorder affecting the autonomic nervous system, leading to symptoms such as rapid heart rate, lightheadedness, and fatigue upon standing. Dr. Cynthia delves into the intricacies of POTS, offering clarity on its diverse manifestations and the challenges involved in diagnosis. POTS affects the autonomic nervous system and can cause dizziness, rapid heart rate, fatigue, and brain fog. However, symptoms vary from person to person. Because of this, working with a knowledgeable POTS specialist in Burbank is essential for accurate diagnosis and effective treatment.
Who Does POTS Impact? | POTS Specialist Burbank Los Angeles
POTS predominantly affects women and individuals assigned female at birth, particularly those aged between 15 and 50 years. However, it’s important to note that men and individuals assigned male at birth can also be diagnosed with POTS.
Certain stressors can increase the likelihood of developing POTS, including:
- Significant illnesses, such as viral infections like mononucleosis or severe infections.
- Pregnancy.
- Physical trauma, such as a head injury.
- Surgical procedures. Individuals with specific autoimmune conditions, such as Sjogren’s syndrome, lupus, and celiac disease, are also more prone to developing POTS.
Recent studies show that COVID-19 may trigger POTS. According to data from nearly 300,000 patients in the Cedars-Sinai Health System between 2020 and 2022, researchers found a small increased risk of POTS after COVID vaccination. However, the risk was much higher after a COVID-19 infection. In fact, getting COVID-19 was linked to a five times greater risk of POTS than vaccination.
Meanwhile, holistic cardiologist Dr. Cynthia Thaik explains how POTS affects heart health. In this guide, she discusses how POTS can impact cardiovascular function. Most importantly, she emphasizes a holistic approach to managing symptoms and protecting long-term heart health.
History of POTS Explained by a POTS Specialist Burbank Los Angeles
The term POTS was coined in 1993 by a Mayo Clinic research team led by neurologist Dr. Philip Low. However, despite its modern name, the condition itself is not new. Historically, POTS has been described by several terms, including DaCosta’s Syndrome, Soldier’s Heart, Mitral Valve Prolapse Syndrome, Neurocirculatory Asthenia, Chronic Orthostatic Intolerance, Orthostatic Tachycardia, Postural Tachycardia Syndrome, and adrenal fatigue POTS syndrome.
In addition, there is evidence suggesting a connection between POTS and anxiety. For example, both conditions may share symptoms such as palpitations, dizziness, and shortness of breath.
POTS Signs and Symptoms – Guidance from a POTS Specialist Burbank Los Angeles
POTS can manifest suddenly or develop gradually, and its classification is a topic of ongoing discussion. However, most authorities recognize distinct characteristics of POTS Disorder Symptoms, with variations among patients such as adrenal fatigue POTS syndrome symptoms.
Symptoms typically arise immediately or a few minutes after sitting up or standing, with some relief experienced when lying down. The range of symptoms associated with POTS is diverse and varies from person to person, including:
POTS has several possible symptoms, and they vary from person to person. Symptoms include:
- Dizziness or lightheadedness, especially upon standing, prolonged standing, or during extended walks.
- Fainting or near-fainting episodes.
- Disrupted sleep due to chest pain, a racing heart rate, and excessive sweating.
- Forgetfulness and difficulty focusing (brain fog).
- Heart palpitations or a rapid heart rate.
- Exhaustion and fatigue.
- Feelings of nervousness or anxiety.
- Shakiness and excessive sweating.
- Shortness of breath (dyspnea).
- Chest pain.
- Headaches.
- Nausea.
- Bloating.
- Pallor and purple discoloration of hands and feet when positioned below the heart.
POTS disorder symptoms often intensify in certain situations:
- Warm environments, such as hot baths, showers, or on hot days.
- Frequent standing, such as waiting in line or shopping.
- Strenuous exercise.
- Illness, such as a cold or infection.
- Menstruation.
Although the origin of POTS symptoms is physical, sometimes people attribute the symptoms incorrectly to psychological disorders such as anxiety. While some people with POTS Disorder Symptoms have anxiety disorders similar to the general population, POTS is not caused by anxiety.

How Is POTS Diagnosed? | POTS Specialist Burbank Los Angeles
Diagnosis of POTS will generally begin with the physician taking a medical history and performing a physical exam. During this initial evaluation, the physician may perform a tilt table study to assess how the heart rate and blood pressure respond when the body changes positions. Based on the results of the tilt table study along with the patient’s reported symptoms, an accurate diagnosis can often be made.
However, in some instances, the physician may order additional tests to rule out other underlying conditions. For example, these diagnostic tests may evaluate the heart muscle, blood flow through the heart, and any abnormal electrical impulses. One commonly used test is an electrocardiogram (EKG), which is a painless procedure that provides a detailed picture of the heart’s electrical activity and overall function.
In addition, an echocardiogram may be recommended. This non-invasive test uses a transducer to transmit sound waves that bounce off the heart, creating detailed images of its structure and movement. Furthermore, electrophysiology studies may be used to closely examine the electrical system of the heart.
Ultimately, your healthcare provider may suggest additional testing to either confirm a POTS diagnosis or eliminate other possible causes of your symptoms. These tests may include:
In some cases, a physician may order additional tests to rule out other conditions. These tests check the heart muscle, blood flow, and electrical activity. For example, an electrocardiogram (EKG) is a painless test that shows how the electrical system of the heart.
Another option is an echocardiogram. This non-invasive test uses sound waves to create images of the heart and evaluate its structure and function.
In addition, electrophysiology studies may be used to assess the heart’s electrical pathways. Based on your symptoms, your healthcare provider may recommend further testing to confirm a POTS diagnosis or rule out other possible causes.
- Blood and urine tests to identify underlying causes of POTS or conditions that mimic its symptoms.
- TST (Tuberculin Skin Test).
- QSART (Quantitative Sudomotor Axon Reflex Test), measuring autonomic nerves controlling sweating.
- Skin nerve biopsy.
- Autonomic breathing test, evaluating your blood rate and pressure response during exercise.
- Echocardiogram.
- Blood volume assessments with hemodynamic studies.
POTS Syndrome Treatment Options
Healthcare providers use several strategies to manage the symptoms of POTS. POTS Syndrome Treatment is highly individualized based on your symptoms and what works best for you. The main forms of treatment include:
- Exercise and physical activity: Studies show that reclined aerobic exercise, such as swimming, rowing and recumbent bicycling, has the best results. Strengthening your core and leg muscles is also helpful.
- Diet and nutrition: If you have the hypovolemic (low blood volume) form of POTS, your healthcare provider will likely recommend increasing both your fluid and salt intake to increase blood volume. Eating a large meal can make symptoms of POTS worse, as your body redirects a lot of blood to aid in the digestion process. Because of this, providers often recommend eating several smaller meals throughout the day instead of two or three large ones.
Medical compression stockings can also help push blood up from your legs to reduce POTS symptoms. They may also give you more endurance to tolerate longer amounts of upright activity before your dysautonomia symptoms set in.
Postural Orthostatic Tachycardia Syndrome (POTS) can be a challenging and debilitating condition for those who experience it. However, it is important to be hopeful and recognize that there are treatment of pots options available that can greatly improve quality of life.
With proper treatment of pots disease, many people with POTS are able to manage their symptoms and live fulfilling lives. This can include lifestyle changes such as increasing fluid and salt intake, exercise, and medications such as beta-blockers or midodrine.
POTS and Hypermobile Ehlers-Danlos Syndrome (EDS)
Some of the symptoms of POTS overlap with symptoms of EDS and HSD. Ehlers-Danlos syndrome is a group of disorders that mostly affect your skin, joints, and blood vessels. People with EDS often have very flexible joints and stretchy skin that bruises easily. According to Standing up to POTS, 80% percent of people with Ehlers-Danlos Syndrome have POTS, and most people with POTS have Type III EDS which is the hypermobility type.
Common symptoms of POTS, Hypermobility Spectrum Disorders (HSD), and Hypermobile Ehlers-Danlos Syndrome (EDS) can vary, but there can be some overlapping symptoms, especially between POTS and joint hypermobility-related conditions.
Here are some common symptoms that may be present in patients with EDS and POTS:
- Lightheadedness or Dizziness: Individuals with both POTS and HSD/EDS may experience lightheadedness or dizziness, especially when transitioning from sitting or lying down to a standing position. This symptom often results from orthostatic intolerance.
- Tachycardia (Rapid Heart Rate): Tachycardia, characterized by a rapid heart rate, is a hallmark symptom of POTS. In some cases, individuals with HSD/EDS may also experience an elevated heart rate, especially upon standing or during physical activity, due to autonomic dysfunction.
- Fatigue: Fatigue is a common symptom in both POTS and HSD/EDS. Individuals with either condition may experience profound fatigue, which can significantly impact their daily functioning.
- Joint Hypermobility: is a feature of HSD and hypermobile EDS. While it’s not a primary symptom of POTS, it can sometimes be present in individuals with POTS, especially those with joint hypermobility-related conditions.
- Chronic Pain: Chronic musculoskeletal pain is frequently reported by individuals with HSD/EDS and can also be a symptom in some POTS patients, particularly if they have underlying joint or connective tissue issues.
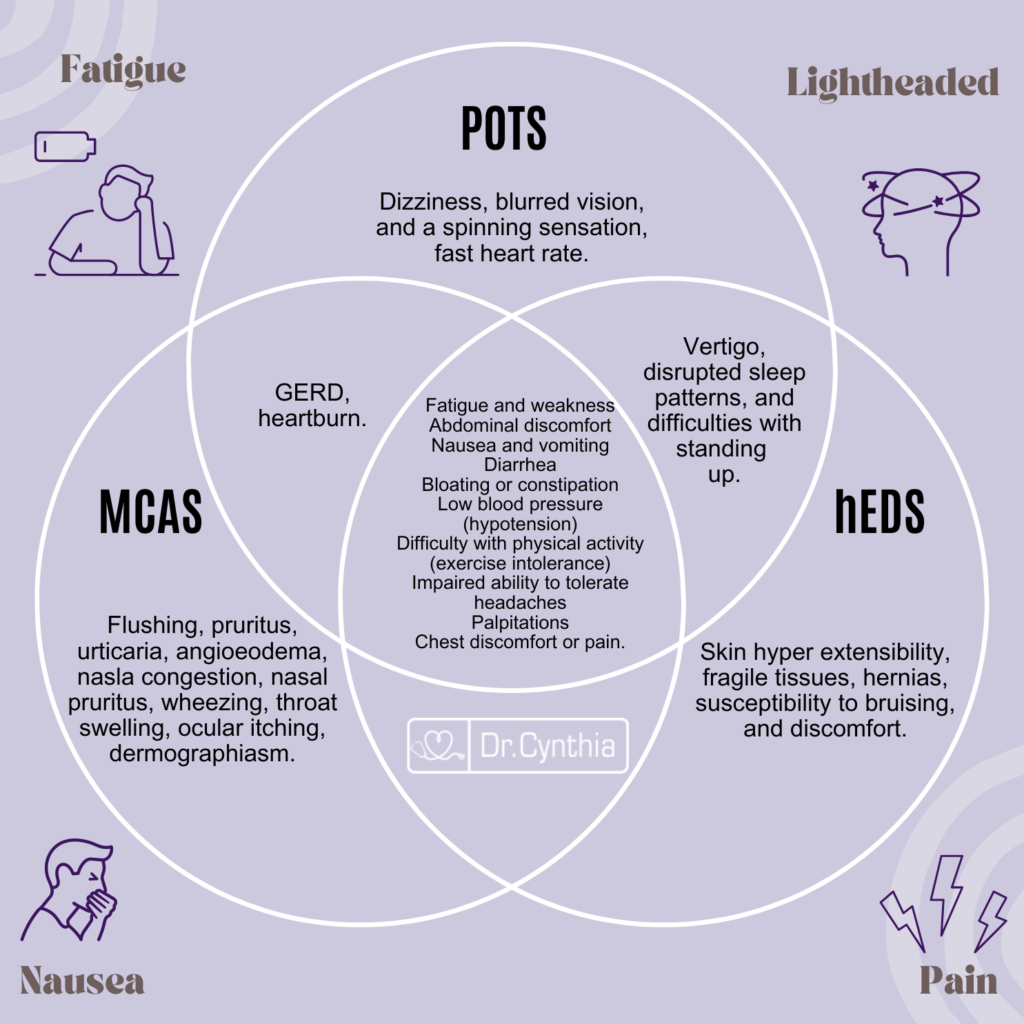
- Autonomic Dysfunction, which affects the autonomic nervous system responsible for regulating functions like heart rate, blood pressure, and digestion, can be present in both conditions. This dysfunction can contribute to symptoms such as sweating abnormalities, digestive issues, and temperature regulation problems.
- Gastrointestinal Symptoms: Gastrointestinal problems, including abdominal pain, bloating, and irritable bowel syndrome (IBS)-like symptoms, can be seen in both conditions due to autonomic dysfunction.
POTS and Mast Cell Activation Syndrome (MCAS
Many individuals with Postural Orthostatic Tachycardia Syndrome (POTS)—especially those with the hyperadrenergic subtype—also experience Mast Cell Activation Syndrome (MCAS). This co-occurrence is more common than previously thought and can significantly complicate both diagnosis and treatment.
Patients with both POTS and MCAS often report symptoms such as:
- Severe flushing or facial redness when standing
- Rapid heart rate (tachycardia)
- Nausea, abdominal cramping, and diarrhea
- Fatigue and brain fog
- Skin reactions like hives or swelling (angioedema)
There is a growing awareness in the medical and patient community that some patients with POTS also have mast cell activation syndrome (MCAS). Mast Cell Activation Syndrome (MCAS – also known as Mast Cell Activation Disorder) is a complex and often underdiagnosed condition where mast cells, a type of white blood cell involved in the immune system, become overly activated, releasing an excessive amount of chemical mediators, such as histamine. This can lead to a wide range of symptoms affecting multiple organ systems. MCAS patients experience recurrent episodes ofanaphylaxis, including symptoms such as hives, swelling, low blood pressure, difficulty breathing, and severe diarrhea. These episodes occur due to the release of high levels of mast cell mediators.
MCAS patients experience repeated episodes of the symptoms of – allergic symptoms such as hives, swelling, low blood pressure, difficulty breathing and severe diarrhea. High levels of mast cell mediators are released during those episodes.
MCAS and POTS can sometimes co-occur in individuals, leading to a more complex clinical picture. The exact relationship between the two conditions is not fully understood, but it’s thought that mast cell activation may contribute to autonomic dysfunction seen in POTS. According to a study published in the Journal of the American Heart Association, MCA disorder is relatively common in patients diagnosed with POTS and who present with additional nonorthostatic gastrointestinal, cutaneous, and allergic symptoms.
What Is MCAS?
Mast cells are a type of white blood cell found throughout the body—particularly in areas like the skin, gastrointestinal tract, and respiratory system. Their job is to defend the body against toxins and allergens. In MCAS, these cells become abnormally sensitive and react excessively to various triggers, releasing inflammatory substances such as:
- Histamine
- Tryptase
- Heparin
- Prostaglandins
- Cytokines
- Free radicals
This release, known as degranulation, leads to symptoms that can resemble allergic reactions and often intensify when the person is upright or experiencing low blood pressure.
How MCAS Affects the Gut and Skin
Mast cell activation can significantly impact the gastrointestinal system. When triggered by certain foods or medications, mast cells in the gut release mediators that:
- Increase fluid secretion
- Trigger smooth muscle contractions
- Cause inflammation and permeability in the gut lining
These responses can result in vomiting, diarrhea, abdominal pain, and food sensitivities. In some cases, antigens from food or medications can also cause skin issues like hives and angioedema.
Why POTS and MCAS Often Coexist
Though the exact mechanism linking POTS and MCAS isn’t fully understood, ongoing research suggests shared pathways involving inflammation, histamine release, and mitochondrial dysfunction. Some experts believe chronic exposure to mast cell mediators like histamine may weaken connective tissue and vascular tone—exacerbating both GI issues and dysautonomia.
In my clinical practice, although literature cites around 9% of POTS patients having MCAS, I find the number to be closer to 50%.
Diagnosis and Advanced Testing for POTS and MCAS
If a patient has persistent gastrointestinal symptoms along with POTS and suspected MCAS, specialized testing is essential. For example, GI biopsy specimens should be stained for CD117, a marker used to identify mast cells. When more than 20 mast cells per high-power field are detected, this strongly supports an MCAS diagnosis.
However, testing alone is not enough. If you experience unexplained gastrointestinal issues, skin reactions, or worsening POTS symptoms, MCAS may be contributing to your condition. Therefore, targeted testing, proper nutritional strategies, and personalized care are important for long-term symptom control.
POTS specialist Burbank – Integrative Care for POTS and MCAS
Dr. Cynthia Thaik, MD is a Harvard-trained holistic cardiologist and a trusted POTS specialist in Burbank. She practices heart-centered, integrative cardiovascular care with a focus on reducing stress, fear, and anxiety while supporting overall well-being.
In addition to conventional care, Dr. Thaik helps patients take an active role in their health through education and guidance. Her team has supported thousands of individuals in making positive changes that improve quality of life.
If you have been diagnosed with POTS or are experiencing related symptoms, a consultation can be an important first step toward managing your heart health. POTS is a chronic condition with fluctuating symptoms and no definitive cure; therefore, treatment focuses on long-term symptom management and gradual improvement.
In treating POTS, Dr. Thaik emphasizes minimizing medication use when possible and focuses on helping patients understand the condition and manage symptoms effectively. Schedule a consultation today to take the first step toward managing your cardiovascular health.
Holistic Strategies for Managing POTS
Dr. Cynthia Thaik’s holistic approach to cardiology also extends to Telehealth POTS consultation and related conditions. Through this approach, the guide outlines holistic strategies that include lifestyle modifications, nutritional support, stress management, and innovative therapies, thereby empowering individuals throughout their healing journey.
Patient-Centered Care at the Holistic Healing Heart Center
At the Holistic Healing Heart Center, patients are at the core of the care paradigm. If you are searching for a Holistic treatment for POTS in Burbank, LA, you need a physician who understands the complexities of this syndrome and can provide a tailored treatment plan to improve your quality of life. Dr. Cynthia Thaik and her team prioritize a patient-centered approach, ensuring that individuals receive personalized care that addresses not only the physical aspects of POTS but also the emotional and spiritual dimensions. If you are searching for a trusted POTS specialist in Burbank, schedule a consultation today to receive personalized and integrative care.
Meet Dr. Cynthia Thaik, MD - Functional & Integrative Cardiologist
Dr. Cynthia Thaik is a board-certified cardiologist who integrates functional medicine into her concierge practice with a specialized focus on cardiovascular and neurovascular optimization.
She devotes one week per month exclusively to functional medicine consultations via telehealth, allowing for deep, unrushed care. During this time, Dr. Thaik works closely with patients seeking transformation, root-cause healing, and individualized strategies grounded in integrative science.
Her approach combines:
- Precision diagnostics
- Advanced cardiovascular expertise
- Compassionate, heart-centered listening
- Extensive patient education
“Cardiovascular consultations and diagnostic services are covered by insurance. Functional medicine services are offered exclusively as concierge, self-pay services”
Schedule Your Telehealth Consultation with Dr. Cynthia
If you’re living with atrial fibrillation and want to explore natural treatment options, Dr. Cynthia is here to help. She provides telehealth consultations to guide you through personalized care plans, addressing lifestyle changes, supplement use, and stress management techniques tailored to your unique health needs.
Dr. Cynthia Thaik will perform a thorough cardiovascular assessment, looking at cardiac function, ruling out structural damage, checking paroxysmal atrial fibrillation symptoms, assessing the adverse effects of hypertension and dietary toxicity (alcohol, caffeine, excessive inflammatory foods), checking for vascular inflammation and endothelial dysfunction, and exploring the impact of stress on arterial tone and the autonomic nervous system regulation of the cardiovascular system.
The patient will have an option to receive individual coaching from a mindfulness instructor. Together, this integrative team approach to Afib will provide the patient with the best opportunity to address the root causes underlying the atrial fibrillation and hopefully restore normal sinus rhythm. As with all health conditions, our goal is to help Afib patients transition from symptoms and disease care to optimal health and wellness – true preventive cardiology.
If you have been diagnosed with Atrial Fibrillation and are looking for natural treatments, Schedule a virtual visit or call for Telehealth Appointment at (818) 842 1410
Frequently Asked Questions
Regular palpitations can be a sign of atrial fibrillation. While this condition can continue for years without harm, a consistent increase in heart rate can cause heart enlargement. This is a hazard which can result in heart failure. Atrial fibrillation also comes with an increased risk of stroke from blood clots that can form as a result.
Without a solid understanding of the causes, it can be hard to definitively put a stop to heart palpitations. However, the treatments mentioned above: reducing stress and intake of stimulants, alcohol, and nicotine, exercising more, and eating a balanced diet, are all good steps forward. If your cardiologist determines that you have a more serious heart condition that may be life-threatening, it will require treatment. There are heart medications which can prevent more serious heart rhythm disorders. However, because of their significant side effects, they are not prescribed lightly. Consequences of misuse can lead to heart attacks, or even sudden death.
Some people experience heart palpitations after eating. While those palpitations may be attributable to an underlying medical condition, it is also possible that the food or beverage that was just consumed is responsible. Sugar can have this effect, particularly on hypoglycemic people. Alcohol is another common influence, particularly among those who have paroxysmal atrial fibrillation (PAF). Foods rich in tyramine or theobromine, such as cheese, red wine, bananas, and especially chocolate (which has both), can increase heart rate and may cause atrial fibrillation.
Actually, no. A more likely cause of heart palpitations is in fact low blood pressure. It is true that medication for high blood pressure can have a side effect of causing palpitations, which may be what is happening when someone with high blood pressure experiences palpitations.